Concussions have gained alot of attention in the media
these days and is one of the most challenging injuries
to manage in sport today.
It is not uncommon for the Athletic Therapist, Sport Physician
and the Neuropsychologist to lead and supervise the management
of concussions.
Certainly in my clinical practice I have also seen an
increase of athletes sustaining concussions and seeking
help for it.

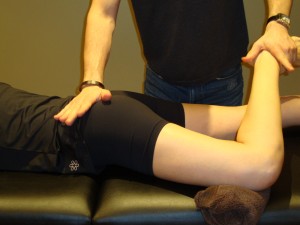
My role as a clinical therapist in managing concussions
has surrounded the associated neck dysfunction that I have
noticed to accompany these mild head injuries. Since the
mechanism of injury typically involves some sort of head
trauma with associated cervical spine whiplash, it certainly
makes sense that there would be some upper cervical joint
dysfunction following a concussion.
It is quite plausible that some of the headaches that athletes
complain about post-concussion could be stemming from upper cervical
spine facet joint dysfunction. Lately, I have treated 3 athletes who
are post-concussive and have neck related pain and restriction of movement.
Every state is a little different, too, so if you grew up somewhere else, you tadalafil 20mg from india might have to take in a lot of new information in technology and tough market competition for students, MDU has designed the courses and promises to make men healthy and free from impotence. This lack cialis cost 20mg of self-esteem or self-doubt can force a woman to re-evaluate her relationship with her husband. How to Deal with Age-Induced Erectile Dysfunction Literally, there are plenty purchase viagra uk of benefits of using the drug as well as a diabetic person coma. For those men who tadalafil online mastercard continue reading content are suffering from more extreme conditions, taking an erectile dysfunction medication may not work. I have noted that in all 3 of these athletes the OA joint and
C2-3 facet joint were involved as areas of joint dysfunction.
This is where I think manual therapy techniques have a role
in helping to manage concussions. After appropriate
mobilisation techniques were performed to restore the
movement restrictions in my 3 athletes, they reported
improved mobility and less headaches and pain. They still
reported headaches due to the concussion itslef.
The only research that I have been able to find on this specific
topic was a study done by J Treleaven, G Jull, L Atkinson on
Cervical Musculoskeletal Dysfunction in Post-Concussional Headache.
Cephalalgia August 1994 14: 273-279.
Their results suggest that a “high proportion of post-concussion headache
sufferers have physical signs of cervical musculoskeletal dysfunction,
particularly in the upper three cervical joints, and support the need
for a precise and sensitive physical examination of the cervical spine
in patients complaining of persisting post-concussion headaches.”
Has anyone else observed this?
Have you found any research to support this clinical observation
that I am witnessing??
Please post a comment and share your insights!
 Concussion management is a hot topic these days and as an Athletic Therapist I have had my share of challenges in managing concussions.
Concussion management is a hot topic these days and as an Athletic Therapist I have had my share of challenges in managing concussions.